Authors: Hoàng Đức Nam, Đào Đức Dũng, Park Young Mok, Chu Chong Woo - Liver, Biliary, Pancreatic Center - Liver Transplantation, Vinmec Times City International General Hospital.
1. Introduction
The indication for liver transplantation is increasingly expanding, and the demand for liver transplants is growing worldwide. Asia is the region with the lowest brain-dead organ donation activity globally, with rates ranging from 0.05-4.04 per million population in 2000, increasing to 0.05-6.0 per million population in 2010; compared to the rates in the US of 22.3 and 17.0 per million population in 2000 and 2010, respectively.[5]
Living donor liver transplantation (LDLT) helps immediately address the shortage of donor organs and was first successfully performed in the world in 1989 with a left liver lobe graft from mother to child [16][19]. Queen Mary Hospital – Hong Kong (May 1996) successfully performed the first adult LDLT with a right liver lobe graft in the world.[13] Subsequently, Asan Medical Center (South Korea, 1997), Kyoto University Hospital (Japan), and the Essen Group (Europe) reported successful implementation of this technique in 1998.[11] Since then, this type of surgery has been increasingly applied worldwide, especially in Asian countries such as Japan, South Korea, Hong Kong, Taiwan... Recent results show that post-transplant outcomes are equivalent to or even better than brain-dead donor transplants [1][9].
In Vietnam, orthotopic liver transplantation has been implemented since 2004, with the first case being a pediatric liver transplant from a living donor.[17] By March 2019, nearly 150 cases had been performed nationwide, with the majority of donors being brain-dead (DDLT) in over 2/3 of cases. We summarize 24 cases of living donor liver transplantation performed at one center in Vietnam (Vinmec Times City).
2. Subjects and Research Methods
24 patients underwent liver transplantation at Vinmec International General Hospital from April 2017 to January 2019. Donors (aged 21-49) had compatible blood types (one case with a different Rh group). Recipients aged 9-66 included 19 males and 5 females.
Patient Selection:
Liver transplantation was indicated for decompensated cirrhosis (with MELD score >15), liver cancer, acute liver failure, and other conditions. Liver cancer was indicated for transplantation within the Milan criteria, with no extrahepatic metastasis. Acute and fulminant liver failure cases were evaluated systemically, with brain CT scans to assess cerebral edema, and MELD Score ≤ 40.
Donor Selection:
Donors underwent strict legal checks, complying with the organ transplantation process of the Vietnamese Ministry of Health, and notifying the National Organ Transplant Coordination Center. After legal confirmation, donor screening involves three stages.
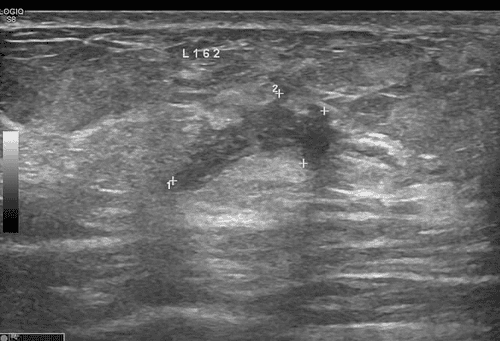
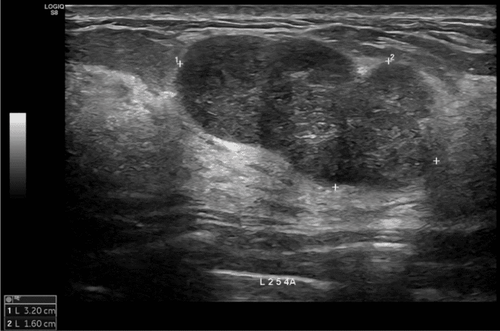
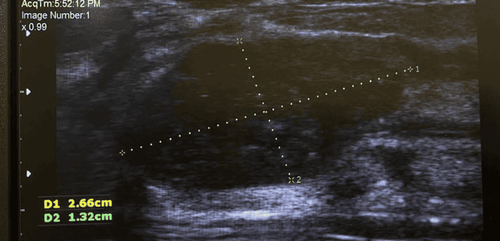
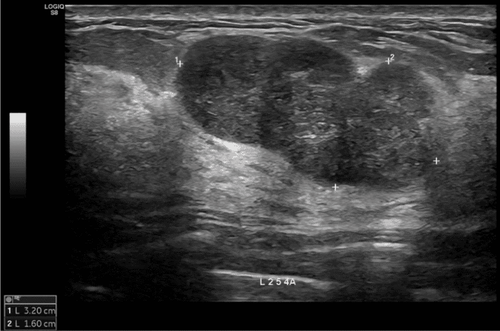
Stage 1: ABO-Rh blood group compatibility; negative HbsAg, Anti HCV, and HIV Ab. Stage 2: Three-phase liver CT scan (measuring volumes of right-left liver regions, reconstructing vascular systems including hepatic artery, portal vein, and hepatic veins. Classifying hepatic artery variants according to Michels, portal vein...); MRI cholangiography to reconstruct the biliary tree. Intrahepatic bile duct variants, especially the confluence of right hepatic ducts according to Hwang et al. [9][18], and assessing liver fat content. Stage 3: Comprehensive testing according to a unified protocol. Donors met requirements when the graft-to-recipient weight ratio (GRWR) ≥ 0.8%; the remaining left liver ≥ 40%, there were no complex anatomical abnormalities of the hilar bile ducts and acceptable liver fat content below 20%.
Standard Liver Volume (SLV) was calculated using the formula SLV = 706.2 x BSA + 2.4 (mL) (BSA – Body Surface Area: total body surface area)[4][20].
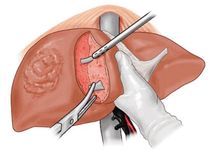
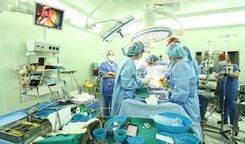
Surgical Method for Donors:
The right lobe graft, including a distal part of the middle hepatic vein, was used in all cases. A J-shaped incision was made below the right rib. Intraoperative ultrasound was used to locate the middle hepatic vein axis, and liver parenchyma was cut using CUSA along this vein axis. Upon reaching the hilar bile duct structures, intraoperative cholangiography was performed to determine the right hepatic duct cut line. The bile duct stump was left 2-3mm, sutured longitudinally to avoid stricture. Methylene blue dye test and intraoperative cholangiography ensured good patency and no bile leakage.
The liver was flushed with 2000mL of cold 4°C Custodiol solution via the portal vein. The right hepatic vein of the graft, along with the middle hepatic vein, was reconstructed into a single orifice using a Goretex vascular graft.
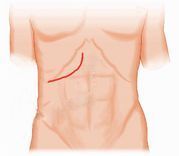
Surgical method for recipients:
In recipients, the diseased liver is completely removed while preserving the inferior vena cava. The right hepatic vein of the graft is connected to the patient's right hepatic vein, extending down to the inferior vena cava. Auxiliary right hepatic veins with a diameter > 5mm are preserved and connected side-to-end to the inferior vena cava. The portal vein is connected end-to-end. Clamps on the hepatic and portal veins are released, and liver reperfusion begins. The right hepatic artery of the graft is connected end-to-end using Sugipro 8/0 under surgical loupes. Intraoperative ultrasound assesses the flow through the connected arteries and veins by measuring flow velocity. Biliary drainage is re-established using either duct-to-duct or hepatico-jejunostomy methods. Cases with two bile duct stumps or when the right hepatic duct is <2mm are internally stented. Methylene blue dye is injected to check, combined with a second intraoperative cholangiography through a bile duct catheter inserted via the gallbladder tube.
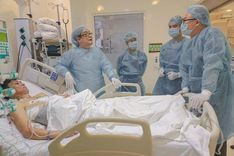
Postoperative care:
Donors are monitored in the recovery room for 1 day. Postoperative pain is managed with paravertebral block anesthesia. Early mobilization, early feeding, and psychological counseling are provided. Liver and bile duct CT scans are performed at 1 week, 1 month, 3 months, and 1 year post-surgery.
Liver transplant recipients receive maximum parenteral nutrition to protect liver cells with appropriate fluid infusion rates. Paravertebral block anesthesia is used for pain management, and early mobilization starts from day 1 post-surgery. Heparin is not routinely used. Immunosuppressive therapy is initiated with steroids, mycophenolate mofetil, basiliximab, tacrolimus, and cyclosporine. For patients with hepatitis B, antiviral tablets and hepatitis B immunoglobulin (Hepabig 2000UI) are used lifelong to prevent hepatitis B recurrence.
Statistical Analysis:
Complications were graded according to the Clavien-Dindo classification[6]. Severe complications of grade III (requiring surgical, endoscopic, or radiological intervention) and grade IV (life-threatening complications requiring intensive care) were recorded and analyzed.
The 1-year survival rate was assessed for patients who had undergone surgery for at least 12 months or had died within 1 year.
Continuous variables are presented as mean ± standard deviation, or median with range.
3. Results
3.1. Table 1. General Characteristics of Patients
4. Discussion
4.1 Overview of Recipients and Donors:
There were 7 genetically related donors, 4 cases related by marriage, and 13 cases confirmed as voluntary donors.
All donor cases had identical ABO blood groups. One case involved a patient with blood type A Rh (-) receiving a liver from a donor with blood type A Rh (+). Post-transplant results showed no abnormalities, and the patient was given additional immunosuppressive agents initially after the transplant.
4.2 Indications for Liver Transplantation
The overall rate of chronic hepatitis B virus infection among our patients was 16/24 (66.7%). There were 6 cases of transplantation due to primary liver cancer (Hepatocellular carcinoma) (5/6 were recurrent cancer after liver resection, TACE, or RFA). 100% of liver cancer cases were related to untreated or inadequately treated hepatitis B virus infection. Six emergency liver transplant cases required plasma exchange and intensive care before surgery (5/6 were acute exacerbations of chronic hepatitis B, 1 case of liver toxicity).
Notably, we performed a liver transplant on a 9-year-old child diagnosed with congenital absence of the portal vein (Abernethy Type I). This is a very rare congenital anomaly worldwide, first discovered and successfully managed in Vietnam.
Emergency liver transplantation for acute liver failure is generally based on King's College and/or Clichy criteria.[10] However, liver transplantation can still be applied to patients who do not meet King's College criteria, as natural recovery is uncertain.[15] In Western European countries, acute and fulminant liver failure is generally prioritized for transplantation in areas with prevalent brain-dead organ donation (liver). Therefore, LDLT is rarely indicated in these centers, based on the need for a larger liver volume than a partial liver graft (right liver) which may not provide the necessary volume to save severely ill liver failure patients, and a rushed screening-evaluation process may lead to inappropriate donor selection. This is a significant difference from many Asian countries, where brain-dead organ donation is still very rare, and living donor liver transplantation accounts for over 90% of cases [1]. Acute liver failure accounts for 5.7% of living donor liver transplantation indications at Asan Medical Center – South Korea, 12% in the Hong Kong research group, and 14.6% according to the Kyoto study [1]. According to Lee SG, at Asan Medical Center - emergency LDLT increased the number of patients needing liver transplantation from 5% to 75%, and the survival rate of acute liver failure patients reached 85% compared to 5% in patients not receiving emergency LDLT.[11]

4.3 Characteristics of Graft Correlation
The volume of the graft relative to the patient's body weight, as well as the quality of the graft (degree of fat degeneration), is significant in predicting post-transplant outcomes. Generally, the graft volume must be over 0.8% of the patient's body weight. In cases of acute liver failure or significant fat degeneration, this ratio requirement is higher. MRI can reliably assess significant fatty liver cases (>15%), often associated with a BMI >25.
Most of our donors were not overweight based on BMI, so we did not routinely perform preoperative liver biopsies. In reality, three donors had a BMI >25, with estimated liver fat content on MRI >15%, and were required to undergo intensive weight loss training for one month. The results showed a reduction in BMI to <22 and liver fat content to <10%.
The smallest remaining left liver volume was 36.7%. The donor recovered well. Centers worldwide suggest limits on the right liver lobe graft with or without the middle hepatic vein (MHV) under different conditions. According to Kyoto University, the graft includes MHV when it is primarily drained by this vein, or when the GRWR is <1%, provided the remaining left liver is over 35%. Chang Gung Memorial Hospital (Taiwan) always includes MHV when the graft is <50% of the recipient's standard liver volume, or when the V5 and V8 veins are large while the right hepatic vein is small.[2] According to Lee S.G (2010), a GRWR of 1% and 0.8% corresponds to a GV/SLF (graft volume to standard liver volume ratio) of 50% and 40%. Graft function assessment shows that most liver failure levels occur with GRWR <1% or GV/SLV <50%.[11] Graft quality can be reflected by liver fat content, ischemia time (clamping the liver pedicle)... According to Fan S.T., with macroscopic fat content over 20%, especially when the remaining left liver volume is <30%, right liver lobe resection for grafting should not be indicated.[7] Our results show safety rates for donors, ensuring sufficient volume, good hepatic vein return, and reasonable portal flow – key issues in living donor liver transplantation using the right liver lobe graft.
4.4 Anatomical Variations of the Right Liver Lobe Graft
According to Lo C.M., the likelihood of encountering abnormal portal vein variations is 10-35% in right liver lobe grafts.[14]. Our study had to change two donors due to type 2 portal vein variations (trifurcation). Accepted liver donors were all identified with type 1 portal veins.

4.5 General Results and Donor Surgery
All our donors were safe, with no deaths and no need for red blood cell transfusions during and after surgery. Many centers also aim to minimize blood transfusions for donors to avoid potential risks associated with transfusions, such as infectious diseases.[7]
Evaluations on three-phase liver CT scans showed that in most cases, segment 4 was drained into both the middle hepatic vein (MHV) and the left hepatic vein. Based on this, in 2/3 of the cases (16/24), we performed an extended right hepatectomy including the MHV. The decision to include or exclude the MHV in the right liver lobe graft depends on the actual anatomical situation and the experience and practices of different centers. The Hong Kong group led by Lo C.M. advocates for including the MHV in the right liver lobe graft.[8][14] At Asan Medical Center in South Korea, 85% of LDLT cases with right liver lobe grafts use an improved technique that preserves the main MHV for the donor, requiring venous reconstruction for the anterior segment using a vascular graft.[11][15]
We encountered one case of obstructive jaundice due to bile duct stricture three weeks post-surgery, which required reoperation to create a bile duct-intestinal anastomosis, with good results. Most other complications were not severe (grade I-II according to Dindo), and patients quickly recovered and improved. Complications and mortality risks in living donors are always a primary concern in living donor transplantation. The larger the liver resection, the higher the risk of liver failure and donor mortality. The mortality risk after left lobe or left liver lobe donation is approximately 0.1%, while it is 0.4-0.5% for right lobe donation. Complications in donors also improve significantly with increased experience at centers. Starting from 1997, by 2002, the annual complication rate at Asan Medical Center decreased from 6.7% to 1.3%.[9][11] A recent multinational study recorded donor mortality and complication rates of 0.2% and 24%, respectively, among 11,553 living donors at 148 centers worldwide.[3]
Most donors could be discharged earlier than the actual time, but some wished to stay longer for convenience in monitoring and caring for the recipient, who is often a family member (child donating to parent, parent donating to the child, etc.). The average hospital stay for donors according to Fan S.T. is 11.5 days (ranging from 6-38 days), with 5 donors wishing to stay longer (over 2 weeks) for similar reasons.[7]
4.6 Surgical Characteristics of Transplant Recipients
The advantage of living donor transplantation is the short cold ischemia time of the organ, which helps maintain the highest quality of the graft. Cases with prolonged surgery times (>10 hours) were due to complex abdominal adhesions from previous surgeries or waiting time for hemostasis before closing the abdomen (due to coagulation disorders in acute liver failure).
4.7 Early Postoperative Results in Transplant Patients
The most common postoperative development in transplant patients is an increase in bilirubin, especially in the first week. This is an initial manifestation of the small-for-size syndrome (SFSS), where the graft is small relative to the recipient's body. This is because most right liver lobe grafts have a smaller volume than required (especially since most liver donors are women while recipients are men), and the graft's hypertrophic proliferation process takes 5-7 days to be effective.[8][14] To address this, besides surgical factors, it is necessary to reasonably limit the infusion volume postoperatively to avoid hepatic congestion and ischemia, and to limit the hypertrophic proliferation of liver cells.[14]
Another common postoperative development is clinical rejection, indicated by a rapid increase in liver enzymes. Our experience suggests using recycling therapy or high-dose steroids (Pulse) when SGOT/SGPT levels rapidly increase above 200U/mL, followed by steroid recycling according to a unified protocol. Except for one case of primary graft non-function, other cases achieved good immunosuppressive results, preserving the graft. According to Lee S.G, living donor liver transplantation (LDLT) has certain advantages, including shortening the cold ischemia time (organ preservation time), thus minimizing graft quality damage. Therefore, the incidence of primary graft non-function is rare, with a frequency of about 0.13%.[4][11]
4.8 Post-Transplant Follow-Up Results
Bleeding at the anastomosis site post-surgery was primarily observed in the first 6 cases, with moderate severity, and was resolved with enhanced hemostasis suturing, achieving good results. Subsequent cases did not encounter significant bleeding complications.
The overall 3-month post-transplant survival rate was 20/24 (83.3%). According to Lee N.R. and colleagues at Samsung Medical Center (South Korea), this rate is 92%. The same authors noted that patients requiring intensive care before transplantation and a MELD Score >35 are two independent risk factors for 3-month post-transplant survival.[12]
The overall 1-year survival rate was 15/19 (78.9%); the 1-year survival rate in the emergency liver transplant group was 4/6 (66.7%). This result is encouraging, as according to Lee S.G, the overall survival rate in the selective - non-emergency group is 73-88%, and the emergency LDLT group is about 50%.[11] Chen C.L and colleagues (2003) also recorded a 1-year survival rate of 78.7 – 97.8% in 5 leading liver transplant centers in Asia during the first 12 years of LDLT implementation, with 1508 patients.[4]
We encountered one case of bile leakage post-transplant, forming a fluid collection at the liver cut surface, which was drained percutaneously (PTD) and healed spontaneously. There were no cases of significant stenosis or thrombosis in the portal vein or hepatic artery. One case of hepatic vein stenosis was successfully treated with stent placement.
Authors Goldolesi (2004), Pomfret (2003), and Kawachi (2002) reported bile duct complication rates ranging from 20 to 40 to 60%[1]. According to Moon D.B., the cumulative bile duct complication rate in LDLT patients after 5 years is 20.2%, mainly bile duct stenosis, most of which were successfully treated with dilation.[15]
3/4 mortality cases were due to severe sepsis, CMV infection, pulmonary and systemic Aspergillus infection, and one case of fulminant liver failure - hepatic coma, hepatorenal syndrome, which was an emergency liver transplant that resulted in death within 30 days post-surgery due to primary non-function graft. Notably, the pulmonary Aspergillus infection cases were related to building renovation and upgrades, despite special isolation measures. This has also been mentioned in the global medical literature.
5/6 of our liver transplant cases for primary liver cancer were recurrent lesions (after liver resection or TACE intervention). One patient developed distant metastasis from the 7th month post-transplant (shoulder bone, pelvic peritoneum), underwent two surgeries to remove pelvic metastasis, and received radiotherapy for the shoulder bone. Notably, this patient also had a history of kidney transplantation from a living donor 5 years prior. Post-transplant liver and kidney function were stable.

4.9 Donor Follow-Up Results
Bilirubin and SGOT/SGPT levels increased post-surgery and mostly returned to normal or acceptable limits within the first week. This result is consistent with the findings of Fan S.T. [7]
Regular follow-up examinations of all donors showed good hypertrophic proliferation of the left liver, averaging nearly 78% of the original liver volume within 3.5 months.
5. Conclusion
Living donor liver transplantation with a right liver lobe graft is still a relatively complex surgery. Thorough screening and appropriate graft selection strategies help ensure the highest safety for donors. After liver donation, the liver recovers in volume and function within 2-3 months, and donors quickly return to normal activities.
For patients needing liver transplantation, this is a high-tech, cutting-edge technique that helps address the severe shortage of donor organs in Vietnam, reducing waiting times and providing more patients with a chance to live.
To arrange an appointment, please call HOTLINE or make your reservation directly HERE. You may also download the MyVinmec app to schedule appointments faster and manage your reservations more conveniently.
REFERENCES: Baker T.B, Caicedo J.C. Chapter 17: Living-donor liver transplantation: indications, outcomes, and surgical considerations; Blumgart’s Surgery of the Liver, Biliary Tract and Pancreas 6th Edition, 2017; pp 1816:33.
Chan S.C., Fan S.T. Historical perspective of living donor liver transplantation. World J Gastroenterol 2008 January 7; 14(1): 15-21.
Cheah YL, Simpson MA, Pomposelli JJ, et al. Incidence of death and potentially life-threatening near-miss events in living donor hepatic lobectomy: a world-wide survey. Liver Transpl 2013; 19: 499-506.
Chen C.L, Fan S.T, Lee S.G, Makuuchi M. And Tanaka K. Living-donor liver transplantation: 12 years of experience in Asia; Transplantation, Vol. 75, S6–S11, No. 3, February 15, 2003, Supplement.
Chen, C.-L. et al. Why does living donor liver transplantation flourish in Asia ? Nat. Rev. Gastroenterol. Hepatol. 10, 746–751 (2013).
Dindo D., Demartines N., Clavien P.A. Classification of Surgical Complications. A New Proposal With Evaluation in a Cohort of 6336 Patients and Results of a Survey; Ann Surg 2004;240: 205–213.
Fan S.T et al. Safety of Donors in Live Donor Liver Transplantation Using Right Lobe Grafts. Arch Surg. 2000;135:336-340.
Hata S. et al. Volume Regeneration After Right Liver Donation; Liver Transplantation, Vol 10, No 1 ( January), 2004: pp 65–70
Hwang S, Lee S.G et al. Lessons Learned From 1,000 Living Donor Liver Transplantations in a Single Center: How to Make Living Donations Safe. LIVER TRANSPLANTATION 2006;12:920-927.
Ichai P, Samuel D. Transplantation hépatique en urgence. EMC Hépatologie 2012;7(1):1-10.
Lee S.G. Living-donor liver transplantation in adults; British Medical Bulletin 2010; 94: 33–48.
Lee N.R, Kim J.M et al. Pre-transplant Predictors for 3-Month Mortality after Living Donor Liver Transplantation; J Korean Soc Transplant 2014;28:226-235
Lo CM, Fan ST, Liu CL, et al. Adult-to-adult living donor liver transplantation using extended right lobe grafts. Ann Surg. 1997; 226(3):261–270.
Lo C.M, Chan S.C. Adult living donor right hepatectomy and recipient operation. Transplantation of the Liver; 3rd Edition 2015, Chapter 50, pp 667-675.
Moon D.B, Lee S.G. Liver transplantation; Gut and Liver, Vol. 3, No. 3, September 2009, pp. 145-165.
Nakamura T, Tanaka K, Kiuchi T, et al. Anatomical variations and surgical strategies in right lobe living donor liver transplantation: lessons from 120 cases. Transplantation 2002;73:1896– 1903.
Nguyễn Quang Nghĩa, Nguyễn Tiến Quyết, Trịnh Hồng Sơn, Đỗ Mạnh Hùng. Ghép gan cho người lớn tại Bệnh Viện Việt Đức, Tạp Chí Y-Dược học Quân sự số Chuyên đề Ghép tạng – 2012, tr.1-7.
Sai V., Raman S.S. Imaging techniques for partial grafting; Transplantation of the Liver; 3rd Edition 2015, Chapter 47 pp 634-641.
Strong RW, Lynch SV, Ong TH, et al. Successful liver transplantation from a living donor to her son. N Engl J Med. 1990;322(21): 1505–1507.
Urata K, Kawasaki S, Matsunami H, Hashikura Y, Ikegami T, Ishizone S, et al. Calculation of the child and adult standard liver volume for liver transplantation. Hepatology 1995;21:1317-21.
Varotti G, et al: Anatomic variations in right liver living donors. J Am Coll Surg 2004; 198:577-582.