This is an automatically translated article.
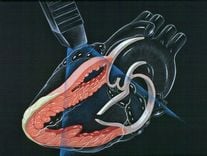
Cardiovascular complications are common after brain injury and are associated with increased morbidity and mortality. Abnormalities included hypertension, hypotension, ECG changes, arrhythmias, release of biomarkers of cardiac injury, and left ventricular dysfunction. Abnormalities are usually reversible and, therefore, management should focus on general supportive care and treatment of the underlying brain injury.Cardiovascular dysfunction is often a complication after a traumatic brain injury resulting in higher morbidity and mortality. Traumatic brain injury leads to dysfunction of the autonomic nervous system (mediated by catecholamines), changes in systemic circulatory homeostasis, caused by nerve stimuli, abnormalities ECG, echocardiography, and changes in serum cardiac enzyme levels (not due to primary cardiac disease). Currently, scientists are still trying to find a way to treat patients with cardiovascular-related complications after traumatic brain injury.
1. What is a traumatic brain injury?
Traumatic brain injury (TBI) affects about 1.8 million people worldwide and it is also one of the main causes of permanent brain damage in exceptional cases.Traumatic brain injury is a disease with a complex pathophysiological process caused by mechanical forces producing physical, cognitive, visual, emotional and sleep disturbances. Traumatic brain injury is also associated with cardiac dysfunction, leading to increased morbidity and mortality in patients because brain function plays an important role in the functioning of the heart through neurological mechanisms. hormones and hormones.
The autonomic nervous system (ANS) forms a complex network in the central nervous system involving structures such as the prefrontal and mediastinal regions of the cerebral cortex, the cerebral amygdala, the terminal striatum, The hypothalamus, perianal gray matter, hemispheres, and medial reticular regions of the medulla are collectively referred to as the “Central Autonomic Network (CAN)”.
The autonomic nervous system, through the sympathetic division, controls the heart and peripheral circuits. In addition, it is important to understand that postionic sympathetic fibers bind to the atria, ventricles, and coronary arteries via the cervical ganglia (upper, middle, and inferior cardiac nerves) or from the thoracic ganglia at the T1 level. – T4, increases heart rate, myocardial contractility and coronary vasodilation. The cardiovascular system is under automatic control known as “neurocardiogenic autoregulation (NCR)”.
Heart rate variability (HRV) has been suggested to assess autonomic variability, reflecting sympathetic and parasympathetic nervous system activity, as a very useful predictor in trauma patients brain injury. Heart rate variability is also a non-invasive electrocardiographic marker that reflects the activity of parts of the autonomic nervous system in the sinus node of the heart, showing the total number of instantaneous heart rate fluctuations and the time in the cardiac cycle.
In addition, this sign indicates an imbalance of afferent and afferent fibers of the autonomic nervous system, causing ventricular tachycardia and sudden cardiac death as well as nervous system control.
Các biến chứng tim mạch thường gặp sau tổn thương não và liên quan đến tăng tỷ lệ mắc bệnh và tử vong
2. Common cardiovascular complications after traumatic brain injury
2.1. Catecholaminergic Effects The hypothalamic-pituitary-adrenal axis works to produce a number of basic hormonally regulated endocrine signals that are integrated with stress sensation, physical performance, and metabolism. At the hypothalamic level, the epigastric nucleus secretes corticotropin-releasing hormone that stimulates the adrenal glands to secrete cortisol. An increase in sympathetic tone induces a catecholamine wave during traumatic brain injury resulting in cardiac damage from hypertrophy and myocardial ischemia.In addition, in the long term, it can cause edema, transient fibrosis, inflammation and necrosis of the constriction band. However, alterations in the hypothalamus and medial cortex alter the central autonomic network, causing adverse cardiac effects. Damage to this area increases the risk of heart complications and can cause blood pressure fluctuations, arrhythmias, and death of heart muscle cells.
2.2. Effects on the circulatory system Moderate traumatic brain injury produces changes in the association between the autonomic nervous system and the autonomic neuroregulatory mechanisms of the cardiovascular system. The degree of delamination is proportional to the severity of the lesions.
Characteristics of catecholaminergic waves include: systemic vasoconstriction followed by increased afterload, cardiac output and oxygen demand, and vasoconstriction (to the coronary circulation) which can lead to myocardial ischemia.
Systemic hypertension also leads to severe pulmonary hypertension, increased hydrostatic pressure, and fluid generation combined with left ventricular dysfunction that can lead to acute lung injury and acute pulmonary edema. A common complication of these cases affecting the lungs is pneumonia, the most common cause of which in these cases is the bacteria staphylococcus (Staphylococcus aureus).
2.3. Heart rate and blood pressure When levels of catecholamines are high, they cause an increase in blood pressure, an increase in heart rate, and an increase in oxygen demand that can lead to submyocardial ischemia leading to impaired ventricular function. However, marked sinus bradycardia occurs due to the baroreceptor reflex (Cushing's triad).
The assessment of the heart's neuroregulatory ability by measuring the heart rate and its oscillations has been put into practice by scientists. The results of the spectral analysis of the heart rate decreased inversely with the severity of the injury and reached zero in the case of brain death.

Khi lượng catecholamine tăng cao, chúng gây ra hiện tượng tăng huyết áp, tăng nhịp tim và tăng nhu cầu oxy có thể dẫn đến thiếu máu cục bộ dưới cơ tim gây suy giảm chức năng tâm thất
These changes are influenced by variables in the natural course of the disease, changes in the areas of injury, and the presence of edema or partial myocardium recovery. These findings and their clinical correlation in the patient's context may establish that it is an acute myocardial infarction (AMI) of coronary artery disease.
3. Diagnosis of common cardiovascular complications after traumatic brain injury
Coronary angiography along with ventricular angiography is considered the gold standard for the diagnosis of cardiovascular complications from traumatic brain injury, although echocardiography is easier to perform and the baseline diagnostic criteria for the latter traumatic brain injury is the apical pitch of the left ventricle. Cardiac enzymes and electrocardiographic findings also have the potential to aid in the diagnosis of cardiovascular complications following traumatic brain injury.Vinmec International General Hospital is equipped with many modern CT scanners such as 512 ranges, 640 ranges, two-energy CT... modern, providing clear images in the body with high accuracy. They have the potential to help doctors eliminate the need for follow-up tests, while also helping patients shorten hospital stays.
In addition, this technology also integrates a shield to regulate radiation exposure. It also prevents unnecessary radiation doses before and after the procedure. With 640-sequence CT scanning technology, the time to record images of the coronary system is only in one beat, significantly reducing image noise caused by movement, so patients can save a lot of time for the examination process. mine.
Please dial HOTLINE for more information or register for an appointment HERE. Download MyVinmec app to make appointments faster and to manage your bookings easily.
Symptoms are not diagnostic criteria as they may be an incidental cause of other reasons, although the symptoms are pre-cardiac pain, shortness of breath or syncope, and a neurological condition. , the patient's debilitated state or body is weakened by a reduced state of consciousness. It should be clarified that cardiovascular complications after traumatic brain injury have been reported to range in severity and may deviate from the definitive diagnosis for this entity due to subjective causes.This explains why so many criteria are needed to make a diagnosis. The Mayo Clinic criteria, since their introduction in 2004 by a panel of cardiologists, have undergone certain revisions to date. The aforementioned echocardiographic findings and the exclusion of coronary stenosis, obstruction, or thrombosis, or concomitant with some other cause of catecholaminergic elevation, such as pheochromocytoma, are diagnostic criteria for Cardiovascular complications after traumatic brain injury.
In addition to these, the InterTAK criteria, which are the result of a global consensus, include possible knowledge of a physical or emotional trigger, a postmenopausal woman's status menstruation and infectious myocarditis.
In addition, the latter criteria do not exclude coronary stenosis but may be a coexisting feature. Comorbidities that may make the application of the above criteria difficult are pheochromocytoma and coronary artery disease. Very similar to these criteria is the Segovia Cubero criterion which divides these harmonizing factors into mandatory, major and minor criteria. There are other criteria such as the Japanese guideline for the diagnosis of cardiovascular complications after traumatic brain injury, which contain many items that may startle the patient about the proprietary nature of the diagnosis.

Một trong những biến chứng phổ biến và nguy hiểm nhất của các ca chấn thương sọ não chính là các biến chứng liên quan đến tim mạch
However, more research is needed to support this view, including complications of cardiac enzyme levels or associated abnormalities and their correlation with overall disease outcome. traumatic brain injury.
Article referenced source: heartmindjournal.org