This is an automatically translated article.
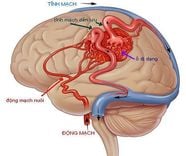
Intracranial hematoma may occur in the brain parenchyma or the surrounding meningeal spaces. Intracranial hematoma or associated potential spaces, including epidural hematoma, subdural hematoma, and subarachnoid hemorrhage. The following article gives us a clear understanding of intracranial hematoma due to traumatic brain injury.
1. What is an intracranial hematoma?
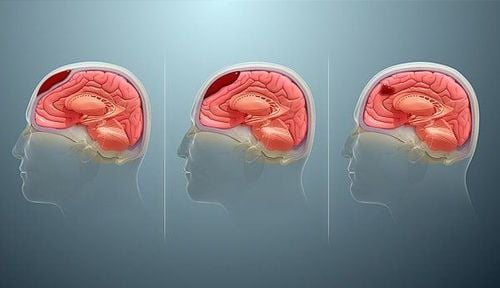
Intracranial hematoma is a collection of blood in the skull. The most common cause is a ruptured blood vessel in the brain or an injury such as a car accident or fall. The blood draw may be in the brain tissue or below the skull, pressing on the brain.
Some head injuries, such as those that cause only a brief loss of consciousness, can be mild. However, an intracranial hematoma is potentially life-threatening. It usually requires immediate treatment, which may include surgery to remove the blood.
2. Causes of intracranial hematoma due to traumatic brain injury
All blood vessels can bleed, but cerebrovascular bleeding is uncommon. If it occurs, there is usually a precipitating factor. Some blood vessels in the brain bleed more easily than others.
Causes of intracranial hematoma and types of bleeding in the brain include:
Head trauma: Any type of head injury, such as from a fall, car accident, sports injury or assault, Both can cause blood clots in the brain. The most common area of bleeding after a traumatic brain injury is between the skull and the surrounding membrane (meninges), which has been described as a subdural hematoma. In addition, head trauma can also increase the risk of stroke. Hemorrhagic Conversion: A cerebrovascular accident is brain damage caused by interruption of blood flow in the brain. An ischemic stroke, which is characterized by insufficient blood flow to the brain, can sometimes cause a hemorrhagic stroke if it is severe and prolonged enough. The process, known as hemorrhagic conversion, usually develops after a blockage of a blood vessel causes it to rupture. Ruptured Aneurysm: A brain aneurysm is an artery that leaks out. It can flare up from malignant hypertension or simply from weakening of blood vessels. This can lead to a subarachnoid hemorrhage, a type of bleeding that occurs underneath the meninges. Subarachnoid hemorrhage usually causes severe headache and loss of consciousness, leading to death in 20 to 50% of cases. Brain Tumor: A brain tumor can cause the area near the tumor to bleed. This occurs when the tumor (and the intracranial pressure associated with it) causes nearby small vessels to thin, rupture, and bleed. Spontaneous bleeding: Rarely spontaneous bleeding in the brain. When it does, the bleeding often affects the cerebral cortex or the inner cyst, causing stroke-like symptoms. A condition known as amyloid vascular disease can end with the use of blood thinners or a bleeding disorder.
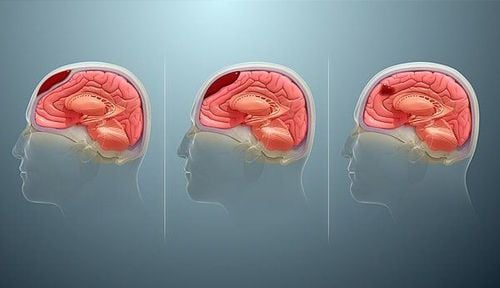
Có nhiều nguyên nhâc khác nhau gây tụ máu nội sọ
3. Classification of intracranial hematoma after traumatic brain injury
3.1. Epidural Hematoma Epidural hematomas can be of arterial or venous origin. Classic arterial epidural hematoma occurs after severe head trauma, typically to the temporal region. They can also occur after a head injury. Typically, a skull fracture with damage to the middle meningeal artery causes arterial bleeding into the epidural space. Although the middle meningeal artery is the artery classically described, any meningeal artery can lead to an arterial epidural hematoma.
Venous epidural hematoma occurs when there is a skull fracture, venous blood from the skull fracture fills the epidural space. Venous epidural hematoma is common in pediatric patients.
3.2. Subdural Hematoma A subdural hemorrhage occurs when blood enters the subdural space, anatomically known as the arachnoid space. Usually a subdural hemorrhage occurs after a blood vessel passing between the brain and the skull is stretched, ruptured, or torn and begins to bleed into the subdural space. These cases most commonly occur after a proximal head injury but can also occur after penetrating or spontaneous head trauma.
3.3. Subarachnoid hemorrhage A subarachnoid hemorrhage is bleeding into the subarachnoid space. Subarachnoid hemorrhage is divided into traumatic and non-traumatic subarachnoid hemorrhage. The second classification scheme divides subarachnoid hemorrhage into aneurysm and non-aneurysm subarachnoid hemorrhage. Aneurysm subarachnoid hemorrhage occurs after rupture of a brain aneurysm allowing bleeding into the subarachnoid space. Non-aneurysm subarachnoid hemorrhage is bleeding into the subarachnoid space without an aneurysm being identified. Non-aneurysm subarachnoid hemorrhage most commonly occurs following blunt trauma to the head with or without penetrating trauma or sudden changes in head velocity.
3.4. Intraparenchymal hemorrhage Intraparenchymal hemorrhage is bleeding into the brain parenchyma. There are many reasons that bleeding can occur such as hypertension, arterial malformation, amyloid angiopathy, ruptured aneurysm, tumor, coagulopathy, infection, vasculitis and trauma.
4. Symptoms of intracranial hematoma
With a traumatic brain injury, signs of an intracranial hematoma appear soon after the head injury or it may take several weeks for them to appear.
However, as time increases, the pressure on the brain also increases, thereby creating the signs of an intracranial hematoma:
Increasing severe headache Nausea and vomiting Consciousness fades , drowsiness, dizziness, anxiety and confusion In the brain and skull, the following symptoms appear:
Bewilderment Unequal pupil size Slurred speech Loss of movement (paralysis) on the opposite side of the body due to a head injury When there is a large amount of blood in the brain When entering the narrow space between the brain and the skull, symptoms such as coma, convulsions, unconsciousness appear.

Tụ máu nội sọ khiến người bệnh đau đầu tăng dữ dội
5. Is blood clot in the brain dangerous?
Intracranial hematoma can be life-threatening and requires emergency care. Seek immediate medical attention after a blow to the head if you:
Loss of consciousness Persistent headache Vomiting, weakness, blurred vision, unsteadiness If signs and symptoms do not immediately apparent after a blow to the head, notice physical, mental, and emotional changes. For example, if someone seems fine after a blow to the head and is able to talk but then loses consciousness, seek immediate medical attention.
Also, even if you feel fine, have someone keep an eye on you. Memory loss after a blow to the head can make you forget the blow. Someone you talk to is more likely to recognize the warning signs and get you medical attention.
6. Prevention of intracranial hematoma
To prevent or minimize head injuries you need to:
Wear a helmet: Wear a suitable and well-fitting helmet when playing contact sports, cycling, motorcycling, skiing, horseback riding , ice skating, skateboarding, snowboarding, or doing any activity that could result in a traumatic brain injury o. Fasten your seat belt: Wear your seat belt every time you drive or sit in a motor vehicle. Protecting young children: Always use properly fitted car seats, table tops and edges, block stairs, fasten furniture or heavy equipment to walls to prevent tipping and prevent children from climbing on objects. not safe. In a nutshell, an intracranial hematoma is a collection of blood in the skull. The most common cause is a ruptured blood vessel in the brain or an injury such as a car accident or fall. Therefore, you need to wear a helmet when playing sports that can lead to head injury, wearing a seat belt when driving or sitting in a motor vehicle.
In order to protect health and prevent complications, when detecting symptoms of memory impairment, severe headache after head injury..., the patient needs to go to the hospital to be treated by a psychiatrist. examination period. Currently, Vinmec International General Hospital is one of the most prestigious medical treatment units for neurological diseases in Vietnam. The Department of Neurology at Vinmec has the function of examining, diagnosing, consulting and treating diseases related to neurological factors, including headaches, cerebellar syndrome, dementia, .. With paraclinical facilities such as electroencephalogram, ST Scan, MRI,...
Neurological examination at Vinmec, customers will be:
Examination by a team of qualified specialists Highly qualified and experienced doctors such as: Doctor Nguyen Thi Minh Phuong, Doctor Bui Ngoc Phuong Hoa, Doctor Vu Duy Dung ... State-of-the-art equipment, comparable to major hospitals in the world: Current operating room greatest in the world ; The most modern silent magnetic resonance imaging machine in Southeast Asia; The 16-sequence PET/CT and SPECT/CT systems help in early detection of neurological damage even when there are no symptoms of the disease. Apply the most advanced intensive treatment techniques in the world in treatment.
Please dial HOTLINE for more information or register for an appointment HERE. Download MyVinmec app to make appointments faster and to manage your bookings easily.